Key Highlights
- Dental implant materials are chosen for their ability to work well with the human body.
- Titanium implants are the most common choice, known for a high success rate and affordability.
- Zirconia implants offer a metal-free alternative, ideal for patients with metal allergies.
- The material for a dental implant can influence its appearance, durability, and longevity.
- Choosing the right material is a key step in replacing missing teeth and restoring your smile.
- With proper care, dental implants can last a lifetime, making them a durable tooth replacement solution.
If you have missing teeth, you understand the impact it can have on your confidence and oral health. Dental implants offer a fantastic, long-term tooth replacement solution that can significantly improve your quality of life.
They look and function just like natural teeth, providing a comfortable and convenient alternative to dentures or bridgework. But have you ever wondered what these advanced artificial teeth are made of? The materials used are key to their success.
In this blog, we will talk about all the materials used in making dental implants, their side effects and advantages.
What Are Dental Implants Made Of?
Modern dental implants are designed using materials that safely integrate with the body while delivering long-term strength. Advances in implant technology have expanded material choices beyond traditional options, allowing dentists to select solutions that balance durability, biocompatibility, and natural-looking results for everyday oral function comfort.
- Titanium implants are widely used for their strength, corrosion resistance, and proven ability to fuse with bone.
- Zirconia implants offer a metal-free alternative with excellent biocompatibility, durability, and natural aesthetics for patients.
Together, these materials make dental implants a reliable, long-lasting solution designed to function and feel like natural teeth.
How Do Implant Components Differ in Material Use?

Implant components vary by material, affecting durability, biocompatibility, cost, and performance. Understanding these differences helps clinicians and patients choose options best suited to functional needs and long-term outcomes for overall success.
1. Titanium Dental Implants
Why Dentists Use Titanium: Dentists prefer titanium because of its exceptional biocompatibility and proven ability to fuse directly with the jawbone through osseointegration. Its unique properties allow strong integration within the implant area, reducing the risk of bone loss and supporting long-term structural stability.
Benefits
- High strength and durability capable of withstanding long-term chewing forces.
- Excellent osseointegration for stable, secure implant anchorage.
- Extensive clinical research supporting safety and minimizing implant failure rates.
- Versatile two-piece designs that allow precise placement of the final dental crown.
Possible Concerns
- Aesthetic Limitations: In patients with thin or receding gums, the metallic tone may subtly show through soft tissue.
- Rare Sensitivity or Allergy: Although uncommon, titanium hypersensitivity reactions have been reported in a very small percentage of patients.
Despite minor concerns, titanium implants maintain success rates exceeding 95% and remain a trusted solution for replacing a missing tooth when supported by proper dental care.
2. Zirconia Dental Implants
Why Dentists Use Zirconia: Zirconia is chosen primarily for its metal-free composition and natural tooth-like color. Dentists often recommend it for patients seeking aesthetic restorations, especially when they are a good candidate with sufficient bone density and healthy surrounding tissue.
Benefits
- White, ceramic appearance blends seamlessly with natural teeth.
- Metal-free option suitable for patients concerned about titanium exposure.
- Low plaque affinity supporting healthier gums and improved patient satisfaction.
- Strong, corrosion-resistant material with favorable biocompatibility.
Possible Concerns
- Design Limitations: Many zirconia systems use single-piece designs, which may reduce prosthetic flexibility during the surgical procedure.
- Long-Term Data: While promising, zirconia has comparatively less long-term clinical research than titanium.
Zirconia implants offer an aesthetic, biocompatible alternative for patients prioritizing natural appearance and modern restorative options.
How Do Dentists Choose the Right Implant Material for You?
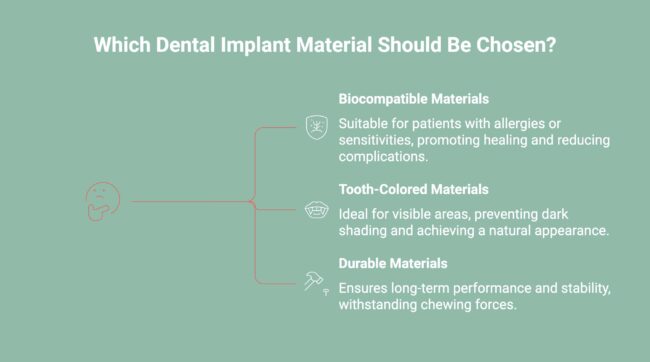
Choosing the right dental implant material depends on a combination of medical, functional, and aesthetic considerations. Each material offers distinct advantages, and the ideal choice varies by patient. Evaluating health history, cosmetic expectations, and long-term performance helps ensure the implant supports both oral function and overall well-being.
1. Allergies, Medical History, and Patient Preferences
A patient’s medical background plays a critical role in selecting implant materials. Known metal allergies, immune-related conditions, or sensitivities may limit suitable options. Some patients also prefer metal-free solutions for personal comfort. These factors often guide dentists toward biocompatible materials that support healing and reduce potential complications.
2. Aesthetic Considerations and Natural Appearance
Aesthetics become especially important when implants are placed in visible areas of the mouth. Gum thickness, tooth position, and smile visibility influence material choice. Tooth-colored materials can prevent dark shading near the gumline and help achieve a more natural-looking result that blends seamlessly with surrounding teeth.
3. Durability, Strength, and Long-Term Performance
Dental implants must withstand daily chewing forces over many years. Material strength, resistance to wear, and long-term stability are essential considerations. Selecting a durable implant material helps ensure consistent performance, reduces the risk of failure, and supports long-term oral health when paired with proper care.
Advanced dental materials, refined through a precise manufacturing process, are designed to mimic a natural tooth, blend with the smile line, and perform reliably during implant surgery and long-term dental implant placement.
Are There Alternative Materials Used in Dental Implants?
Dental implants are no longer limited to a single material. Advances in dental technology have introduced alternatives designed to address allergies, aesthetics, and specific clinical needs, giving patients and clinicians more tailored treatment options today.
Here’s how alternative implant materials compare in practice:
- Titanium Alloys – Long considered the gold standard, titanium provides exceptional strength, durability, and predictable osseointegration with the surrounding jawbone.
- Titanium-Zirconium Alloys (Ti-Zr) – These hybrid alloys enhance mechanical strength while maintaining excellent bone integration, making them suitable for smaller-diameter implants in limited bone volume cases.
- Ceramic-Based Systems – Advanced high-performance ceramics improve tissue response and may reduce inflammatory risks, offering a balance between function and aesthetics.
- Polymer and PEEK-Based Materials – Though less common, polyether ether ketone (PEEK) components are being explored for flexibility and shock absorption in specific restorative applications.
Understanding material alternatives helps ensure implant choices align with biological compatibility, structural demands, aesthetic goals, and long-term treatment expectations.
What Does the Dental Implant Process Involve?
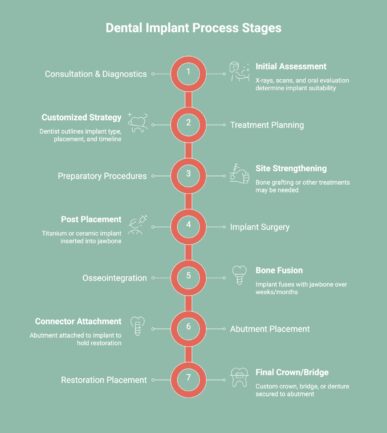
The dental implant process is a multi-stage treatment designed to replace missing teeth with stable, functional restorations. Each phase supports proper healing, bone integration, and long-term success through careful planning and clinical precision.
The implant journey typically includes the following stages:
- Comprehensive Consultation and Diagnostic Imaging: Digital X-rays, 3D scans, and oral evaluations assess bone density, gum health, bite alignment, and overall implant suitability.
- Personalized Treatment Planning: The dentist develops a customized plan outlining implant type, placement location, timeline, and any preparatory procedures required.
- Preparatory Procedures (If Needed): Bone grafting, sinus lifts, or periodontal treatment may be performed to strengthen the implant site before surgical placement.
- Implant Placement Surgery: The titanium or ceramic implant post is surgically inserted into the jawbone to serve as an artificial tooth root.
- Osseointegration and Healing Period: Over several weeks or months, the implant fuses with the surrounding bone, creating a secure and stable foundation.
- Abutment Placement: A connector piece called an abutment is attached to the implant, preparing it to hold the final restoration.
- Custom Crown or Restoration Placement: A precisely fitted crown, bridge, or denture is secured to restore function, appearance, and bite strength.
A clear understanding of each step helps patients prepare mentally and physically for a structured, predictable, and long-term implant solution.
Who Are the Ideal Candidates for Dental Implants?

Dental implants are highly effective, but they are not suitable for everyone. Ideal candidates typically demonstrate good oral health, sufficient bone structure, and habits that support proper healing and long-term implant stability.
Common characteristics of strong implant candidates include:
- Patients with Healthy Gums: Controlled oral conditions reduce infection risk and support long-term implant success following surgical placement and restoration.
- Patients with Adequate Jawbone Density: Sufficient bone structure ensures proper implant integration and long-term stability under everyday chewing forces.
- Non-Smokers or Patients with Managed Lifestyle Factors: Stable health habits improve healing outcomes and significantly reduce complications during recovery.
- Patients Missing One or More Teeth: Individuals seeking a permanent, fixed alternative to bridges or removable dentures often benefit from implant-supported restorations.
- Patients with Fully Developed Jawbones: Adults whose jaw growth is complete provide a stable anatomical foundation for predictable implant placement.
- Patients Committed to Oral Hygiene and Follow-Ups: Consistent brushing, flossing, and routine dental visits are essential for maintaining implant health long term.
Identifying candidacy early allows for realistic expectations and, when necessary, pre-treatment solutions such as bone grafting or periodontal therapy to improve long-term results.
What Should You Consider Before Choosing a Dental Implant?
Choosing a dental implant is both a medical and personal decision. Evaluating functional needs, material preferences, overall health factors, costs, and long-term maintenance requirements ensures informed choices and greater treatment satisfaction.
Key factors to evaluate before proceeding include:
- Material Type and Biocompatibility: Titanium, zirconia, or alloy options differ in strength, aesthetics, and tissue response, which can influence long-term success and comfort.
- Bone Density and Oral Health Status: Adequate jawbone support and healthy gums are critical for proper implant integration and reducing complication risks.
- Treatment Timeline and Healing Period: Implant therapy may require several months, depending on healing speed and whether additional procedures are necessary.
- Total Cost and Financial Planning: Expenses vary based on implant type, diagnostic imaging, surgical complexity, and restorative components.
- Dentist’s Experience and Technology Used: Skilled providers using advanced imaging and surgical planning tools can improve precision and treatment predictability.
- Long-Term Maintenance Commitment: Consistent oral hygiene, routine dental visits, and healthy lifestyle habits directly impact implant longevity and performance.
Careful consideration upfront helps align expectations with outcomes, leading to a confident, well-informed, and successful implant decision.
What Makes Dental Implants at Dentist Tree of the Heights a Trusted Choice in Houston?
At Dentist Tree of the Heights, dental implants are more than just a tooth replacement, they’re a long-term solution designed to restore comfort, function, and confidence. Our team takes a personalized approach, carefully evaluating your oral health, bone structure, and goals to create a treatment plan that feels right for you.
We use modern diagnostic technology and proven implant techniques to ensure precision, safety, and predictable outcomes. From your initial consultation to final restoration, our focus is on clear communication, comfortable care, and results that look and feel natural. Whether you’re missing a single tooth or need a more comprehensive solution, we guide you through every step with transparency and expertise.
Ready to explore your options? Schedule a dental implant consultation at Dentist Tree of the Heights and take the next step toward a stronger, healthier smile, supported by a team you can trust.
Conclusion
Understanding what dental implants are made of is crucial for making informed decisions about your oral health. With various materials available, such as titanium and ceramic, each option offers unique benefits and potential drawbacks. Factors like allergies, aesthetics, and durability play a significant role in choosing the right implant for you. By being knowledgeable about these aspects, you can ensure that your dental implant journey leads to long-lasting results that enhance your smile and confidence.
Frequently Asked Questions
Are there dental implants for people with metal allergies?
Yes. People with metal allergies can choose ceramic dental implants. Zirconia implants are metal-free, highly biocompatible, and designed to avoid allergic reactions. Always discuss material options with your dentist to confirm suitability, safety, and long-term treatment success outcomes.
Is zirconia more durable than titanium for dental implants?
Both zirconia and titanium dental implants are highly durable. Titanium has decades of clinical use and slightly stronger long-term data. Zirconia is extremely strong as well, but has fewer long-term studies due to being a newer implant material.
Have materials for dental implants changed much over the years?
Yes, dental implant materials have changed greatly over time. Titanium was once the standard choice. Advances in technology and manufacturing introduced ceramic options like zirconia, giving patients more biocompatible, aesthetic, and metal-free implant solutions today worldwide in dentistry.
Are there any metal-free options for dental implants?
Yes, zirconia implants are a popular metal-free alternative to traditional titanium implants. Made from strong ceramic material, they offer excellent aesthetics, biocompatibility, and corrosion resistance, making them suitable for patients with metal sensitivities or aesthetic concerns in visible areas.
How do I know if I have titanium toxicity?
Titanium toxicity is extremely rare. Symptoms sometimes linked to sensitivity may include persistent inflammation, unexplained implant discomfort, or allergic-type reactions. Proper medical evaluation, allergy testing, and consultation with your dentist or physician are necessary for an accurate diagnosis.
Are implant crowns glued or screwed in?
Implant crowns can be either cement-retained (glued) or screw-retained, depending on treatment planning and clinical preference. Screw-retained crowns allow easier removal for maintenance, while cemented crowns may offer improved aesthetics in certain restorative situations.
Can you have an MRI scan with dental implants?
Yes, most dental implants, including titanium and zirconia, are MRI-safe and do not interfere significantly with imaging. Titanium is non-ferromagnetic, meaning it does not react strongly to magnetic fields, making MRI scans generally safe for patients with implants.
