Key Highlights
- The dental bone graft creates a strong foundation for dental implants, improving long-term stability and success.
- Multiple dental bone graft materials are used, including autografts, allografts, xenografts, and synthetic options.
- The cost of a dental bone graft usually varies depending on the type of graft material, the complexity of the procedure, and geographic location.
- The dental bone graft procedure involves consultation, site preparation, graft placement, and careful post-operative care.
- Healing occurs in stages, from early tissue recovery to bone integration and maturation, which may take several months.
- Monitoring for signs of failed dental bone graft, such as pain, swelling, or infection, ensures proper recovery.
- The recommended time between graft and implant is usually 3–9 months, with implant placement ideally within 6–12 months.
- Proper care and adherence to the dentist’s instructions maximize graft success and support long-term oral health.
You go in for a routine dental checkup expecting a simple update, but instead, you are told your jawbone has weakened. Suddenly, getting an implant is no longer a straightforward plan. Questions about healing time, treatment steps, and whether your jaw is ready start to feel overwhelming. Missing teeth already affect your comfort and confidence, and now bone loss adds another layer of worry.
That is when the key concern comes up. How long does a bone graft take to heal, and when can you finally move forward with a dental implant? The timing matters because it determines how stable your future implant will be and how soon you can restore your smile.
In this blog, you will get a clear look at the bone graft to implant timeline, factors that influence healing, and the signs that your graft is progressing well. This guide will help you plan your next steps with confidence.
What is a Dental Bone Graft and When Is It Required?
A dental bone graft is a procedure that rebuilds or strengthens areas of your jaw where bone has been lost. Your dentist places safe dental bone graft material into the weak area, and your body naturally forms new bone around it. This helps restore the stability your mouth needs for long-term oral health.
You may need dental bone grafting if bone loss has occurred because of missing teeth, gum disease, or an injury. It is also recommended for bone grafting for implants when the jaw is not strong enough to support an implant on its own. Strengthening the jaw first helps ensure better implant success and fewer complications later.
Not sure whether dentures or implants are right for you? Read our blog on dentures vs implants to understand the differences to make the best choice for your smile.
What Types of Bone Grafts Are Used in Dentistry?

Let us understand the different types of dental bone graft materials that are used depending on the location and amount of bone required.
1. Autografts – Your Own Bone
Autografts use bone taken from your own body, often from the jaw, chin, or hip. Because it comes from you, this type of graft has living bone cells that integrate well and promote faster healing. Autografts are often considered the gold standard for dental bone grafting since they have a high success rate for dental implants and bone graft procedures.
2. Allografts – Donor Bone
Allografts are sourced from human donors and processed in a tissue bank to ensure safety. Using donor bone eliminates the need for a second surgical site, which reduces discomfort. Allografts are commonly used when a moderate amount of bone is required and are a reliable option for patients looking for a safe and effective dental bone graft procedure.
3. Xenografts – Animal Bone
Xenografts come from animal sources, usually bovine bone, and serve as a framework that encourages your natural bone to grow. This type of graft is especially helpful when bone loss is significant. It provides the support needed for successful dental implant and bone graft placement.
4. Alloplasts – Synthetic Bone
Alloplastic grafts are made from synthetic materials such as calcium phosphate or bioactive glass. They are safe, predictable, and avoid any donor site surgery. Alloplasts are an excellent choice for patients who prefer a completely artificial solution without compromising the outcome of dental bone grafting.
5. Composite Grafts – Combined Approach
In some cases, dentists use a combination of graft types, known as composite grafts. For instance, an autograft may be mixed with a synthetic material to enhance volume and support proper dental bone graft healing stages. Composite grafts are ideal for patients who need both strength and a faster healing process.
Each type of graft is chosen based on your dental health, treatment goals, and dental bone graft cost. Knowing your options helps ensure a smooth dental bone graft procedure and sets the foundation for successful implants.
Ready to restore your jawbone and prepare for a successful dental implant? Schedule an appointment with Dentist Tree of Heights.
What Are the Main Types of Dental Bone Graft Procedures?
Different grafting techniques are used depending on the extent and location of bone loss. These are the most common procedures performed to prepare the jaw for implants.
1. Socket Grafts
A socket graft is placed immediately after a tooth extraction. The graft fills the empty socket to maintain bone height and width and prevent early shrinkage. This approach preserves the ridge and keeps the site ready for a future implant.
2. Lateral Ridge Augmentation
Lateral ridge augmentation is used when the jawbone is too narrow to support an implant. Graft material is added along the outer side of the ridge to increase its width. This creates enough space and stability for proper implant placement.
3. Block Bone Grafts
A block bone graft is recommended for areas with significant bone loss. A small block of bone is secured to the weakened area with screws, and the jaw gradually fuses with it. This technique restores both height and width and provides strong support for implants in complex cases.
Together, these procedures address different levels of bone loss and help create the stability needed for successful implant placement. Your dentist will choose the most suitable technique based on the condition of your jawbone and your long term treatment goals.
How Is the Dental Bone Grafting Procedure Performed?
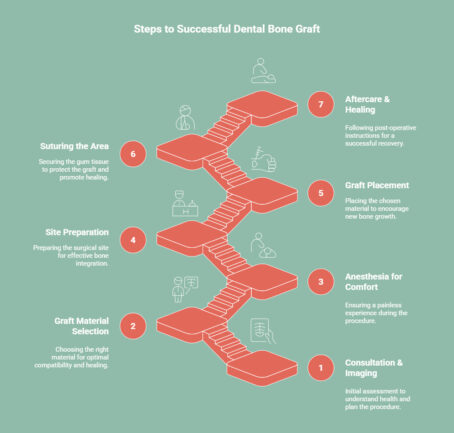
A dental bone graft is carefully planned to ensure comfort, promote healing, and provide a strong foundation for oral health.
1. Consultation and 3D Imaging
Before any surgical work, your dentist will conduct a detailed consultation. This helps them understand your overall health, evaluate the extent of bone loss, and plan the graft procedure precisely. Proper assessment ensures that the treatment is tailored to your needs.
During this visit:
- Your dentist reviews your medical history and oral health.
- Advanced imaging, such as a CT scan, is used to assess bone loss and plan the graft placement.
- The treatment plan, expected outcomes, and potential risks are discussed, giving you an opportunity to ask questions and feel confident moving forward.
2. Selection of Graft Material
Your dentist selects the graft material based on what will create the strongest, most predictable foundation for your implant. The choice typically depends on three key factors:
- Extent and location of bone loss, how much bone needs to be rebuilt and whether the area requires added strength or precision.
- Your healing capacity, including age, medical conditions, medications, and lifestyle habits that influence recovery.
- Timeline for implant placement, whether you need faster integration or have time for a slower, more natural grafting process.
These considerations help determine the material that offers the best stability and long-term success for your implant.
3. Anesthesia for Comfort
To ensure a comfortable experience, anesthesia is used during the procedure. Patients are usually awake but completely numb in the treatment area.
Key points about anesthesia:
- Local anesthesia is commonly used to numb the gums.
- Sedation may be offered for anxious patients to help them relax.
- Modern anesthesia techniques make the procedure virtually painless, allowing your dentist to focus on restoring your oral health.
4. Site Preparation
Once anesthesia takes effect, the surgical site is carefully prepared. Proper site preparation is essential for successful bone integration and long-term stability.
This involves:
- Making a small incision in the gum to expose the jawbone.
- Cleaning and disinfecting the area to minimize infection risks.
- Ensuring a sterile environment so the graft can integrate effectively with your existing bone.
5. Graft Placement
With the site prepared, your dentist places the chosen bone graft material. This step encourages your natural bone to grow into the graft, restoring lost volume and density.
During graft placement:
- The material acts as a scaffold for new bone formation.
- A protective membrane may be used to hold the graft in place and prevent soft tissue interference.
- This stage initiates the dental bone graft healing stages, which are critical for implant success.
6. Suturing the Area
After the graft is in place, the gum tissue is carefully repositioned and secured with sutures. Proper closure supports healing and protects the graft.
Key points about suturing:
- Some sutures dissolve naturally, while others may require removal at follow-up.
- Sutures help stabilize the gum tissue and safeguard the graft material.
- Proper closure ensures a smooth and predictable healing process.
7. Aftercare and Healing
Post-operative care is essential for a successful recovery. Following instructions closely helps minimize complications and promotes proper bone regeneration.
Important aftercare tips include:
- Take all prescribed medications, such as antibiotics and pain relievers.
- Follow a soft diet and avoid putting pressure on the surgical site.
- Avoid smoking and strenuous activities for at least 48 hours.
- Apply ice packs and elevate your head to reduce swelling.
- Maintain gentle oral hygiene and attend follow-up appointments.
Following these steps ensures proper healing and prepares your jaw for future procedures, including bone grafting for dental implants, while reducing the risk of signs of failed dental bone graft.
Discover how dental implants can help seniors regain chewing ability, improve oral health, and enjoy a confident smile at any age.
What Are the Benefits of a Dental Bone Graft?
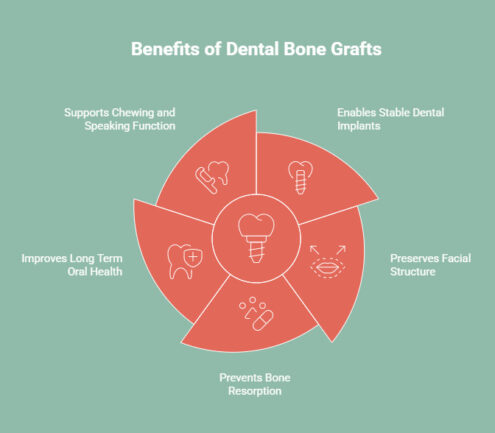
A dental bone graft restores lost bone, strengthens your jaw, and supports both oral health and facial structure. Here are the main benefits of this procedure.
1. Enables Stable Dental Implants
A strong jawbone is essential for successful dental implants. During osseointegration, the implant fuses with the bone, which requires sufficient bone density. If your jaw has experienced bone loss, an implant may fail without a graft.
A dental bone graft rebuilds the bone and creates a solid foundation, increasing the success of your implant. It ensures your future dental implant is secure, durable, and long lasting, making it a key step toward restoring your smile.
2. Preserves Facial Structure
The jaw supports facial muscles and skin. Tooth loss can lead to bone deterioration, which may cause a sunken or aged appearance.
A bone graft restores jaw volume and maintains natural contours in your cheeks and lips. This protects your facial structure, improves appearance, and prepares your jaw for future dental work.
3. Prevents Bone Resorption
Bone resorption occurs when the jaw breaks down bone tissue after tooth loss due to reduced stimulation from chewing. Over time, this can lead to significant bone loss.
A dental bone graft places new bone material, which stimulates growth and signals the body that the area is active. Preventing resorption protects nearby teeth from shifting and avoids more complex problems with jaw structure and oral health.
4. Improves Long Term Oral Health
A restored jawbone supports your remaining teeth, reducing the risk of loosening or shifting. Bone grafts also help manage gum disease by rebuilding damaged areas, stabilizing teeth, and promoting tissue regeneration.
By addressing bone loss early, a dental bone graft strengthens the mouth and supports better oral health for years to come.
5. Supports Chewing and Speaking Function
Jawbone deterioration weakens chewing and can affect speech. A dental bone graft rebuilds the foundation, enabling secure dental implants or dentures.
This restoration allows you to bite and chew effectively and speak clearly, restoring both function and confidence in daily life.
A dental bone graft strengthens the jaw, preserves facial structure, and supports long-term oral health. It is a vital step for restoring function, appearance, and confidence in your smile.
See how all-on-4 implants can replace a full set of teeth using fewer implants and a faster healing process.
What Are The Main Dental Bone Graft Healing Stages?
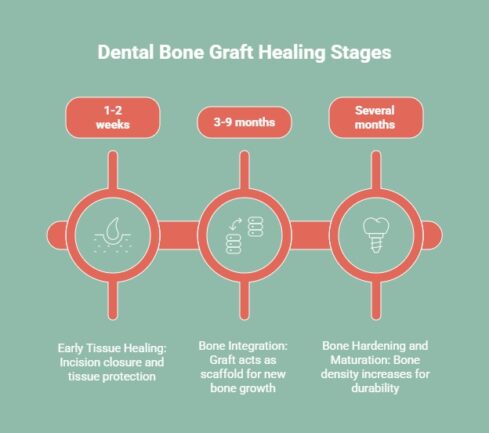
The healing process after a dental bone graft happens in distinct stages. While initial recovery symptoms like swelling and tenderness usually subside within one to two weeks, complete bone healing takes several months. The process focuses on stimulating new bone growth and ensuring the graft fully integrates with your jaw.
1. Early Tissue Healing
The first stage occurs during the initial one to two weeks after your procedure. During this phase:
- The body focuses on closing the incision and protecting the surgical site.
- Swelling, mild discomfort, and bruising are common.
- Gum tissue begins to heal and knit together, forming a protective barrier over the graft.
Proper care during this phase is essential. Maintain oral hygiene with gentle brushing, avoid disturbing the site, stick to soft foods, and refrain from strenuous activity.
2. Bone Integration
After the soft tissue has healed, the bone integration stage begins, usually lasting three to nine months, depending on the graft size and type. Key points include:
- The graft acts as a scaffold for your body’s natural bone-forming cells.
- New bone gradually grows into and around the graft, replacing it with your own bone.
- This process, called osseointegration (especially when preparing for implants), ensures the new bone is strong and stable.
Regular dental check-ups and X-rays allow your dentist to track bone growth and ensure the graft is integrating properly before moving to the next stage.
3. Bone Hardening and Maturation
The final stage focuses on strengthening and maturing the newly formed bone:
- Bone density increases, giving the jawbone the durability needed to support dental implants or other restorations.
- This phase can overlap with bone integration and may continue for several months.
- Your oral surgeon will determine when the bone is sufficiently mature for implants or further dental work.
Once this stage is complete, the grafted bone provides a solid, robust foundation for long-term oral health.
Ready to Restore Your Jawbone and Prepare for Dental Implants? Book your consultation with Dentist Tree of Heights today
What Are the Signs of a Failed Dental Bone Graft, and How Can You Prevent Them?
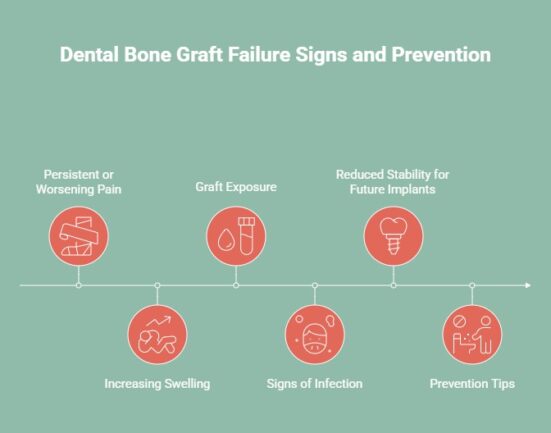
Recognizing warning signs early is essential to protect your oral health and ensure a smooth recovery. Following your dentist’s post-operative instructions remains the most effective way to prevent complications, but knowing what to look for is equally important.
- Persistent or Worsening Pain: Mild discomfort is expected and should improve within a few days. Pain that lasts beyond a week or suddenly increases may indicate infection or improper healing and requires immediate evaluation.
- Increasing Swelling: Swelling normally peaks within 48 to 72 hours, then decreases. If it continues to grow, returns, or appears unusually red or warm, it may signal infection or inflammation.
- Graft Exposure: Seeing a few particles early on can be normal, but visible graft material or gum tissue pulling away from the site is concerning. Exposure increases infection risk and needs prompt assessment.
- Signs of Infection: Watch for pus, fever, worsening pain, persistent bad taste, or foul breath. These symptoms suggest an active infection that can compromise healing and should be addressed right away.
- Reduced Stability for Future Implants: If X-rays show limited new bone growth or ongoing bone loss, the graft may not be integrating properly. A weak foundation can delay or prevent implant placement.
- Prevention Tips: Keep the area clean, avoid strain on the graft, attend follow-ups, and report unusual symptoms early. Careful monitoring helps ensure smooth healing and a stable base for future implants.
Early detection and proper care are key to preventing complications. Always follow your dentist’s guidance to ensure your dental bone graft heals successfully and supports future implants.
What Is the Recommended Time Between a Bone Graft and a Dental Implant?
A dental bone graft typically needs 3 to 9 months to heal and integrate with the jaw, providing a stable foundation for an implant.
Key considerations:
- Optimal Timing: Implants are usually placed 6 to 12 months after the graft.
- Early Placement Risks: Implant stability may be compromised if the bone hasn’t fully integrated.
- Delayed Placement Risks: Waiting too long can cause bone shrinkage, reducing support for the implant.
Sticking to this timeline and attending follow-ups ensures the graft and implant work together for a secure, long-lasting result.
Why Trust Dentist Tree of the Heights With Your Dental Bone Graft and Implants
At Dentist Tree of the Heights, we understand that restoring your jawbone and preparing for dental implants is more than a procedure. It is about confidence, comfort, and long-term oral health. That is why our team combines gentle, compassionate care with advanced technology to make every step of your dental bone graft procedure smooth and stress-free.
Whether you need bone grafting for dental implants, treatment for jawbone loss, or follow-up care during the dental bone graft healing stages, you will receive expert guidance under one roof.
We focus on personalized care and clear communication, helping you understand what is a dental bone graft, your options for dental bone graft material, and how the dental implant and bone graft process works. Our approach ensures you feel informed, comfortable, and confident throughout treatment.
Book your appointment today and take the first step toward a strong, healthy jaw and a smile that lasts a lifetime.
Final Words
A weakened jawbone does not have to stand in the way of a healthy, confident smile. Acting at the right time and following a clear treatment plan can make healing smoother and more predictable. If you are dealing with bone loss or preparing for a dental implant, this is the moment to understand your options and take the next step. With proper care and timely decisions, your jaw can support a strong, stable, long-lasting result.
Frequently Asked Questions
How long does it take to heal after dental bone grafting?
Initial soft tissue healing occurs within 1 to 2 weeks, but complete bone integration takes about 3 to 9 months. Your dentist will monitor progress using X-rays to ensure the graft is fully stable before placing a dental implant.
Is a dental bone graft always necessary before getting dental implants?
Not always. A dental bone graft is needed only if there is insufficient jawbone to support an implant. Your dentist evaluates bone density and decides whether grafting is required to ensure implant stability and long-term success.
Are dental bone grafts considered safe?
Yes. Dental bone grafting is a safe, routine procedure with a high success rate. Biocompatible materials are used, and proper surgical techniques minimize risks, promoting bone growth and supporting long-term oral health and implant success.
How is a dental bone graft procedure performed?
The surgeon makes an incision to expose the jawbone, places the selected graft material, and then closes the gum tissue with sutures. The graft acts as a scaffold, allowing the body to generate new bone over several months.
How painful is dental bone grafting?
The procedure is performed under local anesthesia, so it is not painful. Mild discomfort or swelling may occur during healing, which can be managed with prescribed or over-the-counter pain medication and proper post-operative care.
Is a bone graft necessary for a tooth extraction?
A bone graft may be recommended after extraction if the site is expected to lose bone. This preserves jaw structure, prevents bone resorption, and ensures the area can support future implants or other dental restorations.
How successful are dental bone grafts?
Dental bone grafts have a very high success rate, often near 100% with proper care. Success depends on patient health, post-operative care, and adherence to the recommended healing process to ensure strong bone formation.
What is a dental bone graft?
A dental bone graft is a procedure that adds bone material to areas of the jaw with insufficient bone. It restores volume, strengthens the jaw, and creates a stable foundation for implants or other restorative dental treatments.
